Hello everyone,
Initially, I was going to cover these papers in a reel for my Instagram, but then I realized it was too much information to cram into a short-form video or post, so it turned into a blog post.

First, let’s recap the systematic review and meta-analysis that studied whether immediate dentin sealing (IDS) influences postoperative sensitivity in teeth with indirect restorations.
In this paper, the authors were trying to answer whether Immediate Dentin Sealing would help improve post-op sensitivity after an indirect restoration. They searched for literature on immediate dentin sealing and found 6836 papers. From this number, they narrowed down their search with the following exclusion criteria (the following types of papers were excluded):
- In vitro or ex vivo studies
- Reviews (narrative or systematic)
- Case Reports
- Conference abstracts
- Studies that did not present at least two groups of indirect restorations comparing IDS with DDS
- studies dealing only with direct restorations or comparing indirect restorations with direct restorations
- Studies that compared outcomes between vital and non-vital teeth
- Studies on primary dentition
- Experiments carried out with animal subjects
From 6836 papers, the authors narrowed down the pool to four studies, and only two papers qualified for meta-analysis. The meta-analysis of these two papers showed a very low certainty of evidence that Immediate Dentin Sealing does not reduce post-op sensitivity in teeth restored with indirect restorations.
So to understand the conclusion from this systematic review and meta-analysis, I read the two papers that qualified for the meta-analysis.

ment for postcementation hypersensitivity. Int J Prosthodont. 2010;
23(1):49-52
Here are my notes from the first paper: Effect of immediate dentin sealing on preventive treatment for post cementation hypersensitivity.
Introduction
This study aims to determine whether IDS could reduce or eliminate the occurrence of post-op hypersensitivity in indirect restorations.
Materials and Methods
25 patients: all males between 20-30 years old. They all needed a 3-unit FPD using a mandibular premolar and molar as an abutment. Both teeth are vital. No bone loss or perio. No complaints pre-op to sensitivity
The patients were split into two groups:
Group A: IDS
Group B: no IDS (control)
The adhesive used for immediate dentin sealing is Prime & Bond, a 2-step etch and rinse (5th generation) adhesive system.
Group A:
- Teeth prepped: 2mm occlusal reduction. 1.2mm axial reduction
- Abutment teeth isolated with a rubber dam
- Total etch for 10 seconds.
- Prime & Bond was used on the tooth for 60 seconds. Gentle air for 5 seconds. Cured 20s
- Abutment teeth were temporized
- 3M RMGI was used as the final cement for the final restoration
Group B:
The teeth in group B were prepped, temped and cemented like group A, but “no prime and bond was applied after tooth preparation.” (All they said about group B)
Evaluation:
One evaluator used air from the air/water syringe to determine sensitivity levels. They used cotton pellets to cover the adjacent teeth and blew air over the abutment teeth’s cervical area at a distance of 3cm for 2 seconds. The patients rated the level of sensitivity they had experienced from 0-4.
0= no pain, 1= mild pain, 2= moderate pain, 3 = severe pain, 4 = intolerable pain
The same clinician did the sensitivity test 1 week and 1, 6, 12, and 24 months after cementation.
Results:
Group A experienced statistically less sensitivity than those in group B at 1 week and 1 month after cementation. In contrast, there was no significant difference between Groups A and B at 6, 12 and 24 months after cementation. Teeth in Group A experienced better comfort with the temporary restoration in situ and little discomfort during the cementation appointment.
This study did show some benefits of IDS in the short term. They also included in the discussions that while the teeth were not air tested in the temporary phase, group A had less sensitivity during the temporary phase and less discomfort during the cementation appointment. But some points in this study bothered me.
The material and methods need to describe their protocol for the control group properly. They said, “Group B were prepared with the same standards as Group A, but no Prime & Bond was applied after tooth preparation.” So does this mean they did not even apply an adhesive at cementation and only used the RMGI to cement? Because then, can we say this study compared immediate dentin sealing to delayed dentin sealing (also known as DDS, meaning adhesive was applied at cementation)? Because of these questions, I don’t know if I can take the conclusions of this paper seriously. If the study did not place any adhesive in the control group and only cemented with RMGI, the results show using IDS will decrease sensitivity compared to not using any adhesive at all, but we can’t conclude that IDS will show improved sensitivity compared to DDS where adhesive would have been applied at cementation.

Gresnigt MMM. Randomized clinical trial on the survival of lithium dis- ilicate posterior partial restorations bonded using immediate or delayed dentin sealing after 3 years of function. J Dent. 2019;85:1-10.
The second paper, Randomized clinical trial on the survival of lithium disilicate posterior partial restorations bonded using immediate or delayed dentin sealing after 3 years of function, was written very well and specific about their IDS and control group protocols. Another great detail about this study was that it was a randomized controlled, single-blind clinical trial where each patient received two restorations, one with IDS and the other with delayed dentin sealing at cementation.
Introduction:
Aim: Does IDS affect the survival, success rate, and quality of survival of eMax posterior restorations?
Material & Methods:
Thirty patients were included in the study for 60 restorations on their first or second molars. The preparations were minimally invasive indirect preparations ranging from inlays to onlays and overlays. The restorations were scored from 1-5 on multiple factors of esthetics, function, and biologic properties. Scores were taken at 1 week, 12 months, and 36 months after cementation.
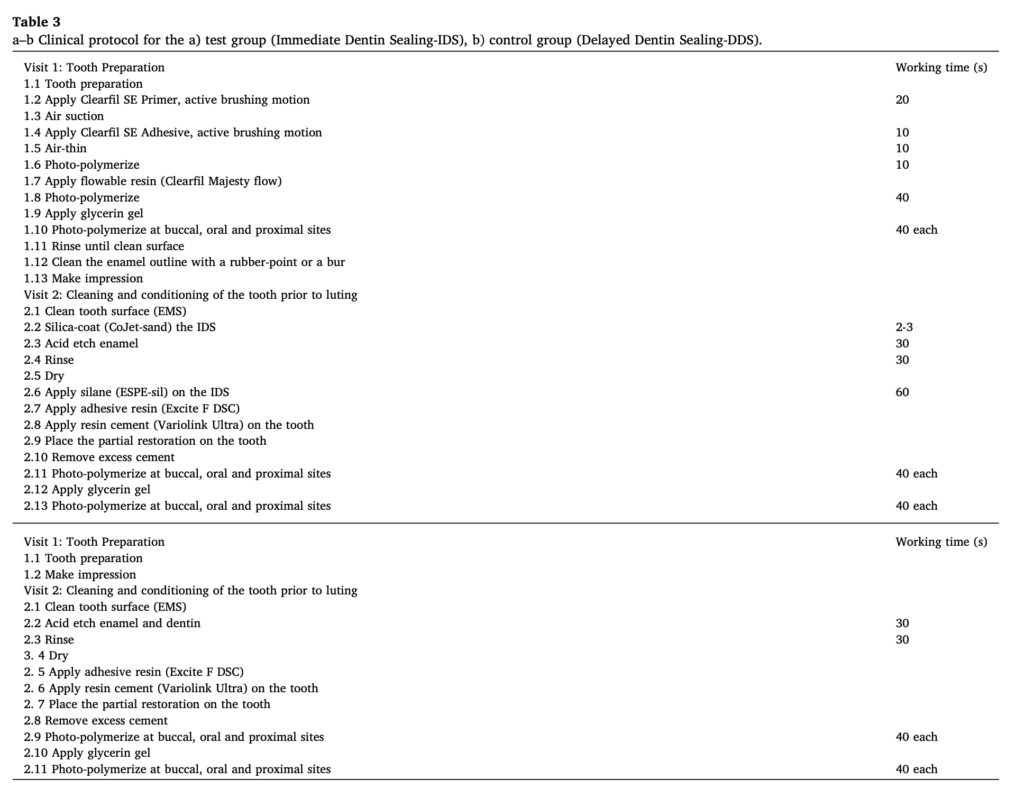
The results found no significant difference in the survival rates between the two groups after three years. A few repairable failures included a debond, wear, chipping, secondary caries, and periodontitis. Only one case was deemed an absolute failure due to deep secondary caries in a medically compromised patient. Five patients experienced post-op sensitivity 1 week after cementation. Still, there was no difference in whether the sensitive tooth had IDS and the sensitivity resolved by 12 months, and there was no reported sensitivity at 36 months in any of the patients.
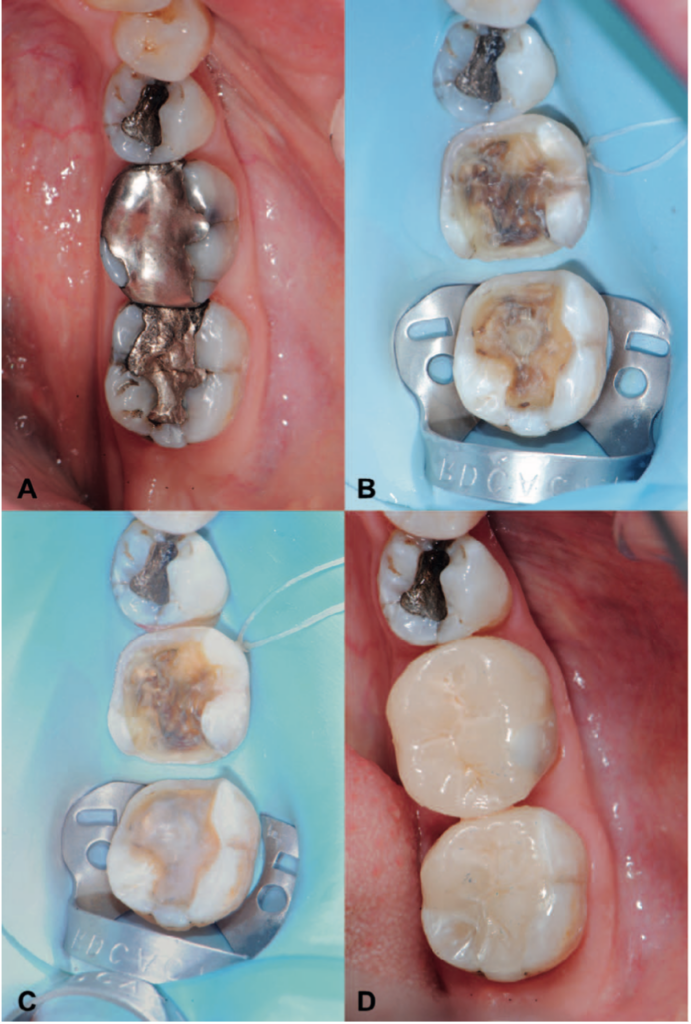
I enjoyed this paper as it was detailed, well-written, and provided documentation of the work and failures. An interesting point in the discussion was that any early failures were due to technique in the procedure. These early failures were not due to the fatigue of the restorations. The thought I had after reading this statement is that three years is too short for us to see whether the Immediate Dentin Sealing will affect the outcome of these restorations and what influences early failures is the clinician’s skill or biological factors from the patient.
As for the post-op sensitivity, the authors wrote in the discussion, “none of the patients complained about post-cementation sensitivity, probably because of the minimal invasive preparation design.” This statement makes sense as these minimally invasive prep designs have less dentinal exposure than traditional crown preparation.
Remember, sudden movement of fluid that causes dentinal sensitivity. As long as we do not create gaps large enough to cause this rapid movement, we will not experience sensitivity due to our bonding procedure. Placing IDS right after preparation means these tubules are sealed and stopping the movement of fluid, which will then decrease sensitivity issues. Even if you do not use IDS and do not create a situation where this fluid will rapidly flow, you will not have sensitivity. This is why the results can be inconsistent. I will always do IDS because using this technique guarantees no fluid movement, and as a clinician, you will have greater control over your outcomes. And as a control freak, I love the predictability that IDS has given me in analyzing post-op sensitivity that may occur in my work because there are more than bonding errors that can cause post-op sensitivity.
If you want to read about post-op sensitivity, check out my blog post on this subject!
Thank you for reading my thoughts on these two papers. Let me know what your thoughts are in the comments!
Hi doc ,for me ids definitely changed post op sensitivity complains after indirects ,since started i only had one patient complain of sensitivity during provisional and that patient had an extraction next to the abutment so some
Cementum ended up being exposed after prep and retraction ..otherwise with onlays ,inlays i leave my patients without temporary ,just the bio-base and none complained of sensitivity even though most of them had very deep carious lesions ..so me too ..will always use ids becasue the least of the benifits is the short term reduction of sensitivity and during temporisation is BIG DEAL for patients 👍
Hi Dr Ashley
Beyond post op sensitivity, IDS has the benefit of greater bond strenght in Indirect restorations
Another possible cause of post op sensitivity may be how we use our handpieces
And the amount of water we use while working
Greetings from Caracas 😉